D7950: Major Ridge Augmentation Billing and Clinical Guide
Dental practices often face challenges when documenting for advanced bone grafting procedures. If you are searching for D7950, you might be dealing with a case that demands coding accuracy, clear documentation and careful insurance management.
The D7950 dental code represents a major grafting procedure of the mandible or maxilla. It is used to rebuild significant bone height or width, often in preparation for dental implants or for correcting trauma, cysts, or tumor defects. Unlike minor grafts or socket preservation, this code includes harvesting bone, graft placement, and the use of both autogenous or non-autogenous materials.
It is important to understand dental code D7950 to comply, minimize denials and ensure predictable dental insurance reimbursement. Following ADA CDT coding guidelines makes sure that the procedure is documented and billed correctly.
Key Takeaways:
-
D7950 is a major ridge augmentation code for the mandible or maxilla, but it must be well documented and have radiographic evidence.
-
Differentiating D7950 vs d7953 and following payer-specific policies reduces the number of denials and ensures accurate dental insurance reimbursement.
-
Correct handling of D7950 claims improves dental revenue cycle management and protects practice revenue.
What Is the D7950 Dental Code?
The D7950 dental code is defined under CDT code D7950 as an osseous, osteoperiosteal, or cartilage graft of the mandible or maxilla. This is a per-arch billed procedure and often involves significant reconstruction of jawbone height or width. In contrast to the minor grafts, D7950 is used for major ridge augmentation, often required months after the tooth extraction, to prepare the site for dental implants or repair defects which may have been caused by trauma, cysts or tumours.
The procedure includes several important steps:
-
Harvesting autogenous or non-autogenous graft material
-
Placement of the graft into the affected jaw area
-
Obtaining and molding the material as needed
Autogenous grafts use bone from the patient, while non-autogenous grafts can be allograft, xenograft, or synthetic. Each step must be properly documented to comply with clinical documentation standards and for successful dental insurance reimbursement.
You should remember that D7950 is not meant for routine, minor grafting or immediate socket preservation following tooth extraction. The improper use of this code can result in claim denials and delays. Understanding its scope and reporting requirements helps in accurate billing and improved revenue cycle performance.
At Meds Dental, we assist practices to properly code D7950 dental code, reducing claim denials and ensuring more predictable reimbursement.
Clinical Scope & When to Use D7950
The D7950 dental code is used for major bone grafting in the mandible or maxilla when considerable ridge augmentation is needed. It is used to restore bone height and width to support dental implants or repair defects caused by trauma, cysts, tumors or severe periodontal loss.
This code is applicable to both autogenous grafts and non-autogenous grafts. Surgical documentation and radiographic evidence for claims are necessary to have successful dental insurance reimbursement.
Usually, D7950 procedures are performed months after tooth extraction so that sufficient healing can occur. Understanding its clinical indications minimizes claim denials and complies with CDT code D7950 standards and ridge augmentation reimbursement guidelines.
D7950 vs D7953 - Key Differences
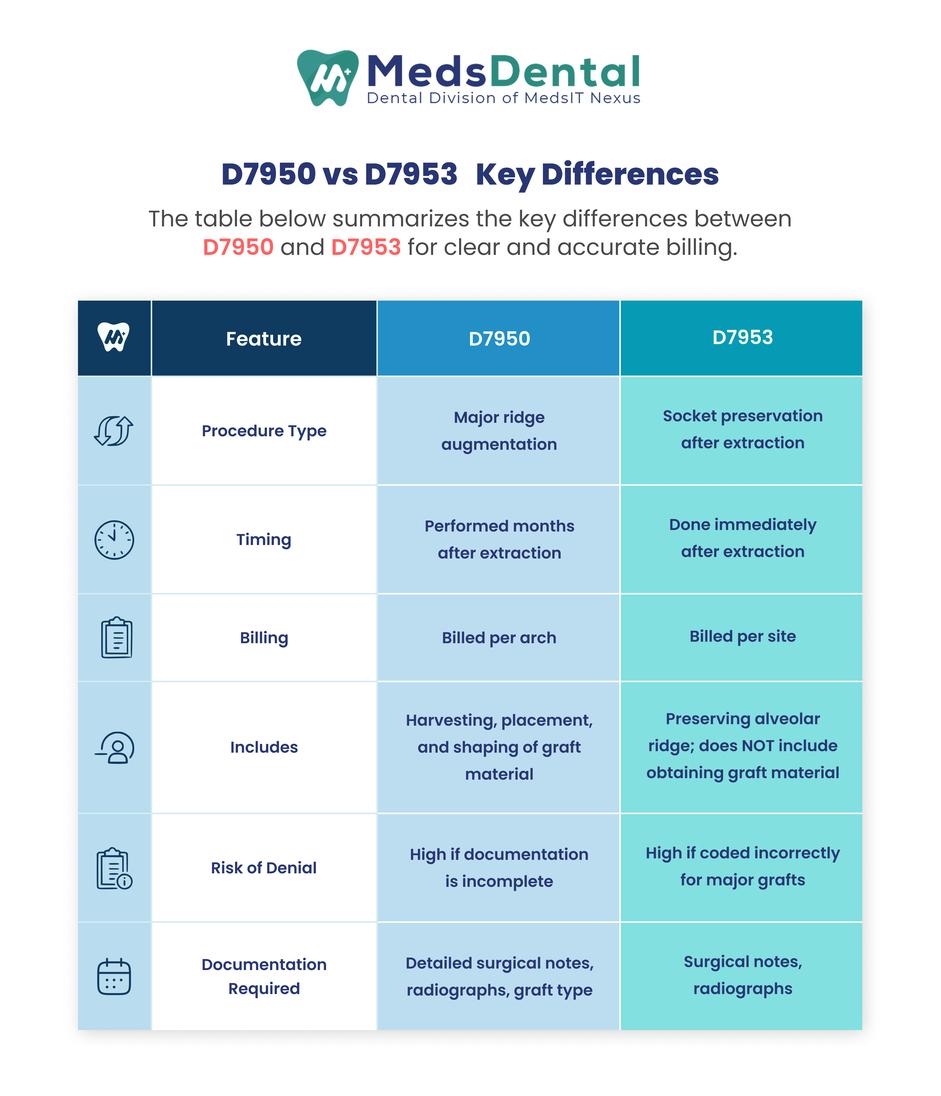
The table below summarizes the key differences between D7950 and D7953 for clear and accurate billing.
|
Feature |
D7950 |
D7953 |
|
Procedure Type |
Major ridge augmentation |
Socket preservation after extraction |
|
Timing |
Performed months after extraction |
Done immediately after extraction |
|
Billing |
Billed per arch |
Billed per site |
|
Includes |
Harvesting, placement, and shaping of graft material |
Preserving alveolar ridge; does NOT include obtaining graft material |
|
Risk of Denial |
High if documentation is incomplete |
High if coded incorrectly for major grafts |
|
Documentation Required |
Detailed surgical notes, radiographs, graft type |
Surgical notes, radiographs |
By following clinical documentation standards and adhering to oral surgery CDT codes 2026, dental practices can reduce denials and ensure smooth dental revenue cycle management.
Documentation & Claim Submission Checklist
Accurate documentation is important when billing the D7950 dental code. Every claim must state the clinical necessity for major ridge augmentation, including the site, extent of bone loss, and type of graft material used. Detailed surgical notes and radiographic evidence for claims help justify the procedure to payers.
Following D7950 documentation checklist assists practices in meeting payer requirements and securing approvals efficiently.
-
Clinical narrative that explains the procedure
-
Indication and diagnosis for major ridge augmentation
-
Type of graft (autogenous or non-autogenous)
-
Surgical technique and procedural details
-
Pre- and post-operative imaging
Dental practices should also verify insurance coverage before surgery and ensure all claim submission requirements are met. Following payer-specific policies and documenting in accordance with clinical documentation standards supports a smoother claim adjudication process and improves dental insurance reimbursement outcomes.
Insurance Coverage & Reimbursement Challenges
Insurance coverage for D7950 can differ widely across PPO, Medicaid, and other insurance plans. Many payers demand clear justification of medical necessity documentation before they can approve major ridge augmentation procedures. Lack of documentation or insufficient radiographs leads to partial reimbursement or claim denials.
Dental practices should remain aware of reimbursement limitations, frequency limitations, and coverage differences between in-network provider billing and out-of-network reimbursement. Pre-authorization and accurate coding save time and ensure dental insurance reimbursement is as high as possible
Understanding payer requirements and staying compliant with ADA CDT coding guidelines safeguards practice revenue. Effective management of D7950 claims can significantly improve dental revenue cycle management and prevent costly mistakes.
Common Denials and How to Prevent Them
Many claims for D7950 dental code are rejected due to missing or incorrect documentation. Common causes include a lack of clinical narrative, inadequate radiographic evidence to support claim, or using the incorrect code for the procedure. Misunderstanding the distinction between D7950 and D7953 also leads to frequent denials.
To reduce denials, dental practices should make sure that all required information is well-documented.
Revenue Cycle Impact for Dental Practices
Billing D7950 accurately has a direct impact on a practice’s financial health. Inadequate documentation or coding mistakes may slow down the reimbursements and increase accounts receivable days.
Dental revenue cycle management can be improved by adhering to ADA CDT coding guidelines and by using oral surgery billing codes properly. Clear documentation, pre-authorization, and accurate submission reduce denials and enhance cash flow.
Effective handling of D7950 dental code claims not only ensures reimbursement but also enhances compliance and patient trust. Optimized revenue cycles make high-value procedures like major ridge augmentation financially sustainable for dental practices.
With Meds Dental, handling D7950 dental code claims is simplified, improving dental revenue cycle management and safeguarding practice revenue.
Frequently Asked Questions:
1. What is the D7950 dental code used for?
The D7950 dental code is used to report an osseous, osteoperiosteal, or cartilage graft of the mandible or maxilla that restores significant bone volume. It applies when extensive ridge augmentation is needed to support implants or repair jaw defects, and the code is submitted with a narrative “by report.”
2. How is D7950 vs d7953 different?
D7950 covers major ridge augmentation and includes harvesting and placing graft material, whereas D7953 is for socket preservation immediately after extraction and does not include obtaining graft material. Confusing the two often leads to claim denials.
3. Is D7950 insurance coverage in the USA guaranteed?
Coverage for D7950 varies by payer. Some dental plans exclude it as a dental benefit, requiring medical plan review, while others may cover it with thorough medical necessity documentation and imaging support.
4. What documentation is needed for a D7950 claim?
Successful claims should include diagnosis, surgical notes, graft type (autogenous or non‑autogenous), and appropriate radiographic evidence for claims. Missing documentation is one of the most common reasons for denials.
5. Can D7950 be billed with implant placement?
Many payers do not allow D7950 dental code to be billed on the same date as implant placement. It must be supported by a clear clinical timeline and justification to avoid reimbursement issues.

.jpg)


.jpg)
